Cervical Cancer Treatment
Comprehensive diagnosis, personalized care, and advanced therapies by Dr. Manish Singhal.
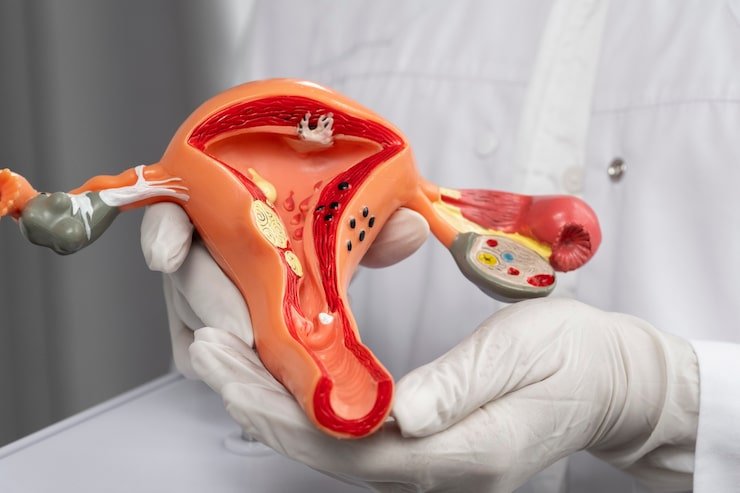
Understanding Cervical Cancer
Cervical cancer is the term used to depict tumors that can develop at the lower end of the womb. These tumors typically create from anomalous cell changes at the passageway to the womb from the vagina (the opening of the cervix). Irregular cell changes can be recognized through screening and after that expelled. An immunization against infections that reason growth (HPV antibody) can diminish the danger of cervical disease. The cervix (neck of the womb) is a solid, strong tube-like structure. The exceptionally base end of the cervix stands out into the vagina a bit, at the opening of the cervix. Within the cervix is fixed with a mucous layer. Organs in the mucous film create a thick fluid (cervical bodily fluid) that goes about as an obstruction, keeping germs from entering the womb from the vagina.
Most cervical cancers (80 to 90 percent) are squamous cell tumors. Adenocarcinoma is the second most normal sort of cervical cancer, representing the rest of the 10 to 20 percent of cases. Adenocarcinoma creates from the organs that deliver bodily fluid in the endocervix. While less regular than squamous cell carcinoma, the frequency of adenocarcinoma is on the ascent, especially in younger women.
Cervical cancer is the second most common tumor for ladies around the world, but since it creates after some time, it is additionally a standout amongst the most preventable sorts of disease.Cancer of the cervix has a tendency to happen amid midlife. Half of the ladies determined to have the infection are in the vicinity of 35 and 55 years old. It once in a while influences ladies under age 20, and around 20 percent of judgments are made in ladies more seasoned than 65. Consequently, it is imperative for ladies to proceed cervical cancer screening until at any rate the age of 70.
There are several treatment plans for cervical cancer patients, even during the Covid-19 pandemic. Some oncologists are altering treatment plans, and some are postponing treatment. Dr. Manish Singhal , the best cancer specialist in Delhi NCR and Oncologist in Noida and his team are taking a different route by providing cancer care services while maintaining safety measures including chemotherapy at home, video consultation, online check-in, and more. Dr. Singhal is trusted by thousands of patients for the best treatment on Cervical Cancer in Noida.
What Causes Cervical Cancer?
Knowing the root causes helps in better prevention and early intervention.
HPV Infection
Sexual action with somebody who has HPV is the most well-known way somebody gets HPV.
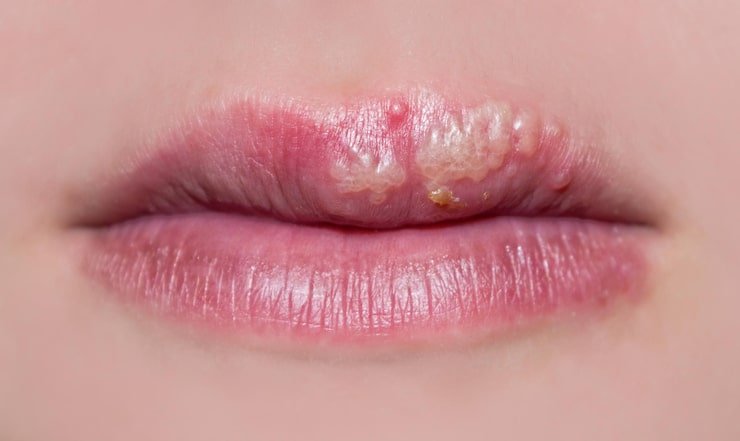
Herpes
Women who have genital herpes have a higher danger of having cervical cancer.

Smoking
Ladies who smoke are twice as liable to create cervical cancer as ladies who don’t smoke.

HPV Infection
Sexual action with somebody who has HPV is the most well-known way somebody gets HPV.

Herpes
Women who have genital herpes have a higher danger of having cervical cancer.

Smoking
Ladies who smoke are twice as liable to create cervical cancer as ladies who don’t smoke.
Common Signs & Symptoms
Know the common indicators that should never be ignored.
Symptoms: Pelvic pain, irregular vaginal discharge, unusual vaginal bleeding, and urinary leakage are common indicators of pelvic or gynecological issues. These symptoms can arise from infections, hormonal imbalances, weakened pelvic muscles, or other underlying conditions. Experiencing any of these signs warrants medical evaluation to identify the cause and ensure timely treatment.

Pelvic Pain
Persistent or intermittent discomfort in the lower abdomen or pelvic region, which may indicate underlying gynecological issues.
Irregular Discharge
Changes in the color, consistency, or amount of vaginal discharge, sometimes accompanied by odor, which may signal infection or hormonal imbalance.
Vaginal Bleeding
Unusual bleeding outside of the normal menstrual cycle, including spotting or heavy bleeding, which could be a sign of conditions like fibroids, hormonal changes.
Urinary Leakage
Involuntary urine release, often during coughing, sneezing, or physical activity, indicating possible pelvic muscle weakness or incontinence.
Pelvic Pain
Persistent or intermittent discomfort in the lower abdomen or pelvic region, which may indicate underlying gynecological issues.
Irregular Discharge
Changes in the color, consistency, or amount of vaginal discharge, sometimes accompanied by odor, which may signal infection or hormonal imbalance.
Vaginal Bleeding
Unusual bleeding outside of the normal menstrual cycle, including spotting or heavy bleeding, which could be a sign of conditions like fibroids, hormonal changes.
Urinary Leakage
Involuntary urine release, often during coughing, sneezing, or physical activity, indicating possible pelvic muscle weakness or incontinence.
Staging for Cervical Cancer
Understanding how cervical cancer is classified helps determine the right treatment and predict outcomes.
In Stage 1 cervical cancer, the disease is confined entirely to the cervix — it hasn’t spread to nearby tissues or lymph nodes. At this stage, the cancer cells are growing only in the surface layer or deeper tissues of the cervix.
It’s often discovered through a Pap smear or HPV test, sometimes even before symptoms appear.
Common treatment options include surgery (like a hysterectomy), cone biopsy, or laser therapy, depending on how deep the cancer has grown. Since it’s still localized, the chances of full recovery are very high when treated promptly.
In Stage 2, the cancer has moved beyond the cervix and uterus but hasn’t reached the pelvic wall or the lower part of the vagina. It might start invading nearby tissues, such as the upper part of the vagina or the area around the uterus.
Symptoms such as abnormal vaginal bleeding, pelvic pain, or unusual discharge may become more noticeable at this stage.
Treatment usually involves a combination of surgery and radiation therapy, sometimes paired with chemotherapy to destroy remaining cancer cells. The disease is still considered treatable and potentially curable if detected and managed early.
At Stage 3, cervical cancer has spread further within the pelvic area. It may have reached the lower third of the vagina, the pelvic wall, or nearby lymph nodes, potentially blocking the flow of urine from the kidneys to the bladder (a condition called hydronephrosis).
Symptoms may intensify, including persistent pelvic pain, back pain, swelling in the legs, and difficulty urinating.
Treatment usually includes radiation therapy combined with chemotherapy (chemoradiation). Surgery is less commonly an option at this stage due to the cancer’s spread. The main goal here is to control the disease and relieve symptoms.
Stage 4 represents the most advanced phase of cervical cancer. The cancer has spread beyond the pelvic region to distant organs such as the bladder, rectum, lungs, liver, or bones. This stage is divided into:
Stage 4A: Cancer spreads to nearby organs like the bladder or rectum.
Stage 4B: Cancer reaches distant organs (metastasis).
Symptoms can include fatigue, weight loss, severe pelvic pain, blood in urine or stool, and chronic back pain.
While this stage is more difficult to cure, advanced treatments — such as targeted therapy, immunotherapy, and palliative care — can help control symptoms, slow progression, and improve quality of life.
Emotional and psychological support, along with medical care, becomes a vital part of the treatment plan.
How Cervical Cancer is Diagnosed?
Modern diagnostic tools enable early detection and better treatment planning.
Pap Smear Test
HPV Test
Colposcopy
Biopsy
Advanced Treatments for Cervical Cancer
Cutting-edge treatments offering renewed hope and longer, healthier lives.
The treatment procedure depends on several factors, which include the type, stage, grade and also the symptoms and the patient’s overall health. The doctor will go through everything related to your health, be it your health history or your present health and will recommend the treatment accordingly.
Below are some tests and procedures which will be a part of your treatment.
Surgery remains one of the most effective treatment options, especially in the early stages of cervical cancer.
A Hysterectomy involves removing the cervix and uterus, and sometimes nearby lymph nodes, to prevent the cancer from spreading.
A Radical Hysterectomy may also remove parts of the vagina and surrounding tissues if the cancer has invaded deeper layers.
For women who wish to preserve fertility, a Trachelectomy (removal of the cervix but not the uterus) can be performed in selected early-stage cases.
Minimally invasive techniques, like laparoscopic or robotic-assisted surgery, are now commonly used to reduce recovery time and complications.
Chemotherapy uses anti-cancer drugs to kill rapidly dividing cells or stop them from multiplying. It’s often used in combination with radiation or as the main treatment in advanced and recurrent cervical cancer.
Commonly used drugs include cisplatin, carboplatin, paclitaxel, and topotecan.
Chemotherapy may cause side effects like nausea, hair loss, or low blood counts, but advances in supportive care have made these effects more manageable.
In many cases, it helps shrink tumors before surgery or control cancer spread when surgery isn’t an option.
Radiation therapy uses high-energy X-rays or other particles to destroy cancer cells. It is often recommended for stages 2 and beyond or when surgery isn’t possible.
There are two main types:
External Beam Radiation Therapy (EBRT): Delivers radiation from outside the body to the pelvic region.
Brachytherapy: Involves placing a radioactive source directly inside or near the tumor.
It’s often combined with chemotherapy (chemoradiation) to enhance effectiveness. Side effects can include fatigue, skin irritation, or mild bladder and bowel discomfort, which are usually temporary.
Targeted therapy focuses on specific molecules or pathways that cancer cells use to grow and survive.
The most commonly used targeted drug in cervical cancer is Bevacizumab (Avastin), which works by cutting off the tumor’s blood supply (anti-angiogenesis therapy).
This treatment is often combined with chemotherapy for advanced or recurrent disease, improving survival rates and reducing tumor progression.
Unlike traditional chemotherapy, targeted therapy causes less harm to normal cells, making it a more precise and personalized treatment option.
Immunotherapy helps the body’s own immune system recognize and destroy cancer cells.
Drugs like Pembrolizumab (Keytruda) — a PD-1 inhibitor — are used when the cancer has spread or recurred after other treatments.
This approach boosts immune responses against cancer cells that often hide from the immune system.
Ongoing research is introducing newer immunotherapy combinations that show promising results in improving patient survival and quality of life.
For advanced stages, palliative care focuses on relieving symptoms such as pain, fatigue, or emotional distress.
It’s not just end-of-life care — it’s an essential part of improving comfort, mental well-being, and overall quality of life during and after treatment.
Counseling, physiotherapy, and nutritional guidance are also provided to help patients cope better with the side effects of intensive treatment.
Patient Success Stories
Inspiring stories from patients who fought cancer and won.



Can cervical cancer be prevented?
Yes, through regular Pap smears, HPV vaccination, and practicing safe sex, the risk can be significantly reduced.
Is cervical cancer curable?
When detected early, cervical cancer is highly treatable and curable. Advanced stages may require combined therapies for effective control.
What age should women start screening?
Screening typically starts at age 21 and continues regularly as advised by healthcare professionals.
Does HPV infection always lead to cervical cancer?
No, most HPV infections clear naturally. Only persistent high-risk HPV infections can cause cervical cell changes leading to cancer.
